Specialty Surgeries / Procedures
Dr Seth Has Experience With The Following Specialty Surgeries
(**Dr Seth is not a boarded specialty surgeon**)
(He has taken a special interest in continuing education and hands on experience to provide these surgeries at a more affordable price when the cost of the specialist is prohibitive)
.png)
TPLO
ACL Repair
Our dogs are more frequently experiencing ACL (Cruciate Ligament) tears. There are 3 common ways to surgically repair an ACL tear. Two are ideally done with a specialist ($$$)- the TPLO and TTA.
Dr Seth performs a modified lateral suture technique. He has successfully corrected over 600 dogs with this technique. With the new line technology, it can be reliably utilized in pets from 10lbs to 150lbs.
If your pet has been diagnosed with an ACL tear and want an option more cost conscious than the TPLO/TTA- contact us and we can discuss your options.

TTA
FHO (Femoral Head Osteotomy
There are times when dogs and cats are in need of a salvage procedure when there is a traumatic or degenerative process going on with their ball and socket joint. In dogs, hip dysplasia and chronic arthritis are the two most common pre-dispositions.
In cats a femoral head/neck fracture and arthritis are most common.
This procedure is the alternative to a total hip replacement. It removes the offending painful ball from the socket joint and a "false joint" is created. The pet can still run and play and maintain quality of life after this procedure.
.jpg)
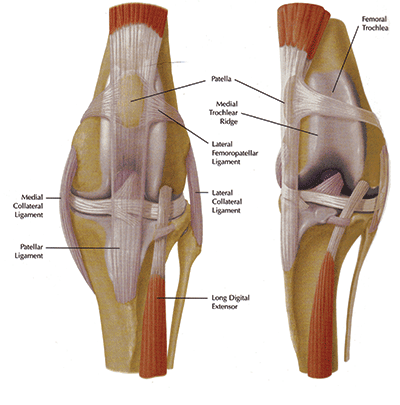
Patellar Luxation
At this time I offer a medial release/lateral imbrication for Grade 1-2 patella luxations. Grade 3 and higher generally need a more invasive surgery to correct and I plan to take continuing education courses to offer further surgical options for pets that suffer from this condition.

Pin/Cerclage Fracture Repair
Dr Seth is able to repair certain bone fractures that can be reduced using IM pins, cerclage wire, and Kirschner pins.
If a fracture is deemed to need a plate and screws - he refers to his Purdue classmate Dr Thomas Hitzeman in Auburn.
Other Procedures
+PRAA (Persistant Right Aortic Arch
+Simple External Hepatic Shunt Constrictor Ring Application
+PDA (Patent Ductus Arteriosus)
+Episioplasty (For hooded/recessed vulva)
+Splenectomy
+Bladder Stones (Cystotomy)
+Intestinal Surgery (Resection/Anastamosis)
+Simple oblique fracture reduction (pin and cerclage)
+Diaphragmatic Hernia Repair
+Open chest lung abcess/cyst removal
+Perineal Urethrostomy
+Thyroidectomy
+Partial Mandibulectomy
+Eye Enucleation
+Amputation
